What is an auscultation: definition, technique, and clinical significance
What is an auscultation?
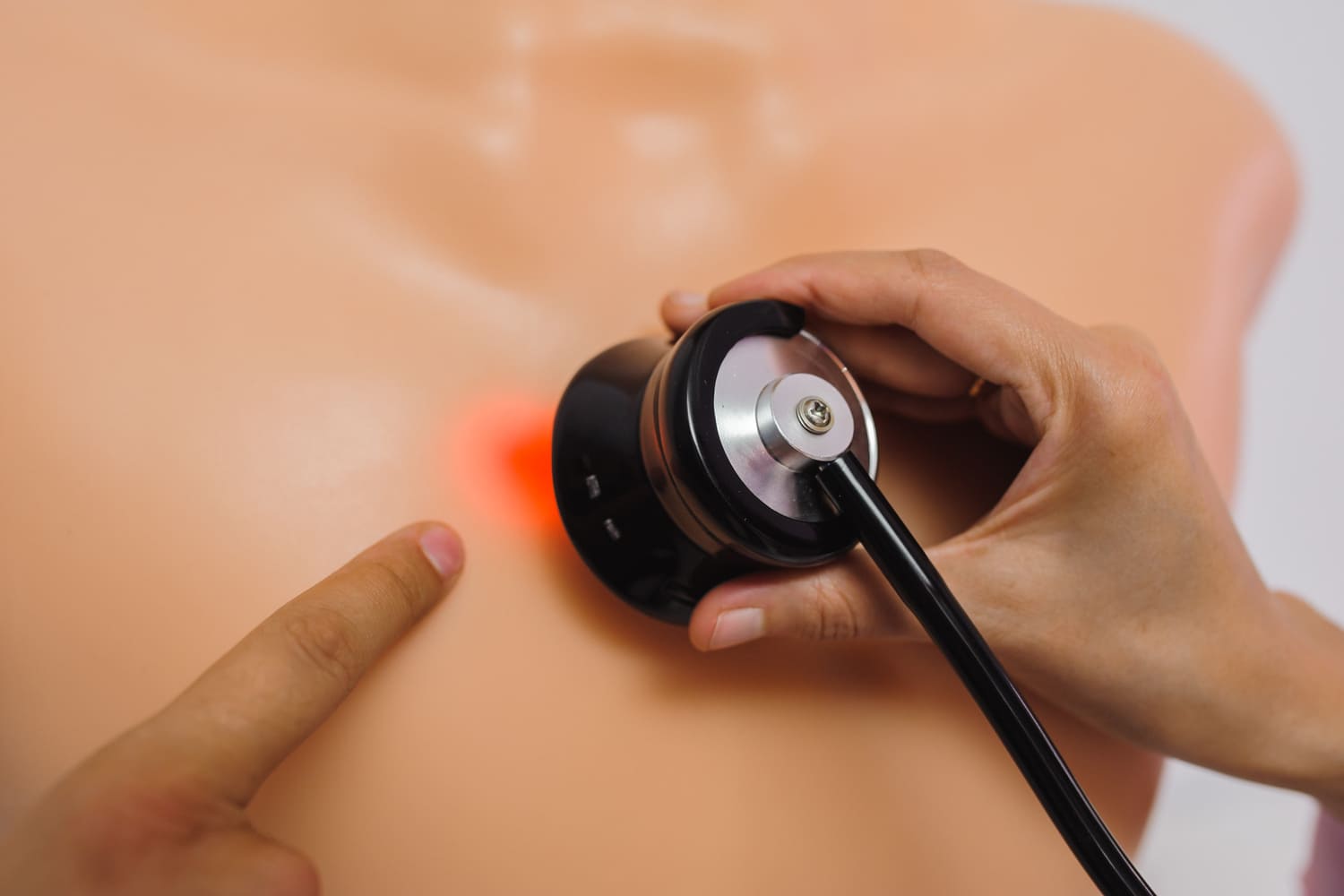
What is an auscultation? Auscultation is a medical examination method based on listening to internal body sound produced by the heart, lung, and other organs using a stethoscope. It is performed to evaluate physiological and pathological changes within the respiratory system, cardiovascular system, and abdominal region.
In clinical practice, auscultation focuses on identifying normal and abnormal sound patterns. These sound signals help clinicians assess airflow, cardiac rhythm, vascular flow, and intestinal activity. The interpretation of sound variations forms the foundation of diagnostic reasoning in bedside examination.

Why is auscultation important in medical assessment?
Auscultation remains a core component of physical examination because it provides immediate information about internal body function without invasive procedures. Through careful listening, clinicians detect subtle changes in sound that may indicate early disease.
In medical school, students develop auscultation skills as part of foundational training. These skills are refined during clinical rotations where repeated exposure to normal and pathological sound improves diagnostic accuracy.
Key clinical purposes of auscultation include:
- Evaluation of heart sound and rhythm
- Detection of abnormal breath sound
- Assessment of vascular flow
- Monitoring of gastrointestinal sound
How is auscultation performed?
Auscultation is typically performed using a stethoscope placed on specific anatomical landmarks. Proper technique ensures accurate transmission of sound from the internal body structures to the examiner.
The process involves:
- Identifying correct anatomical zones
- Ensuring minimal external sound interference
- Systematic listening to compare bilateral regions
- Interpreting variations in intensity, pitch, and duration of sound
During cardiac assessment, heart sound patterns such as S1 and S2 are analyzed. In pulmonary evaluation, clinicians assess breath sound, airflow distribution, and abnormal respiratory noises.
What types of sound are evaluated during auscultation?
Different organs produce characteristic sound patterns. Understanding these variations is central to effective auscultation skills.
Heart sound
Cardiac auscultation focuses on normal heart sound, murmurs, gallops, and additional acoustic events. Each sound corresponds to mechanical activity within the cardiovascular system.
Lung and respiratory sound
Pulmonary auscultation evaluates lung expansion and airflow. Clinicians assess normal vesicular breath sound and identify abnormal respiratory noises such as wheezes, crackles, or diminished sound transmission.
Abdominal sound
Bowel activity produces characteristic intestinal sound. Abnormal patterns may indicate obstruction or reduced motility within the digestive system.
Auscultation skills in nursing and medical education
Auscultation skills are developed through structured training and repeated clinical exposure. In medical school and nursing programs, students learn to differentiate normal from pathological sound patterns.
Nurse auscultation training emphasizes systematic listening, anatomical accuracy, and correlation between sound findings and patient symptoms. Through simulation-based education, students practice interpreting sound in controlled environments before applying these skills in clinical settings.
Simulation tools such as MATT (Auscultation) and Pediatric MATT are designed to support the development of auscultation skills by reproducing realistic heart sound, breath sound, and other clinical audio scenarios. These training solutions allow learners to refine diagnostic listening without patient risk.
Clinical interpretation of auscultation findings
Accurate auscultation requires not only detecting sound, but understanding its clinical meaning. Changes in sound quality may reflect structural, inflammatory, or functional conditions.
For example:
- Altered heart sound may indicate valvular dysfunction
- Reduced breath sound may suggest airway obstruction
- Added respiratory noise can signal fluid accumulation
- Absent intestinal sound may reflect decreased motility
Because interpretation depends on experience, continuous practice strengthens auscultation skills.
Limitations of auscultation
Although auscultation provides immediate diagnostic insight, it is subjective and dependent on examiner experience. External sound interference, improper technique, or limited training may reduce accuracy.
For this reason, structured education and standardized nurse auscultation training improve consistency. Modern simulation-based learning environments enhance reliability in identifying clinically significant sound variations.
Historical development of auscultation
Auscultation as a clinical method was systematized in the early nineteenth century, when structured listening to internal sound became part of formal medical examination. Since then, auscultation has remained a central diagnostic tool in bedside assessment.
Despite technological progress in imaging and laboratory diagnostics, the interpretation of sound from the body continues to support immediate clinical decision-making. The historical evolution of auscultation skills demonstrates how structured training improves diagnostic reliability.
The physics of sound in auscultation
Understanding how sound travels through the body enhances the accuracy of auscultation. Internal sound is generated by vibration—valve closure in the heart, airflow in the lung, or movement within the digestive system.
During auscultation, these vibrations are transmitted through tissues to the chest wall, where they are captured and amplified. Differences in tissue density affect how sound is perceived. For example, fluid accumulation alters normal respiratory sound transmission.
A clear grasp of acoustic principles strengthens auscultation skills, especially in complex clinical scenarios.
Systematic comparison during auscultation
Effective auscultation is based on structured comparison. Clinicians assess symmetrical areas of the body, comparing sound intensity and quality between right and left sides.
In pulmonary assessment, comparison of bilateral breath sound helps identify localized abnormalities. In cardiac examination, evaluation of multiple valve areas allows interpretation of subtle changes in heart sound.
This systematic approach is emphasized in both medical school curricula and structured nurse auscultation training.
Common errors in auscultation interpretation
Even experienced clinicians may misinterpret sound findings if technique is inconsistent. Errors in auscultation may occur due to:
- External environmental sound
- Improper stethoscope placement
- Incomplete comparison of anatomical zones
- Overreliance on isolated sound events
Developing advanced auscultation skills requires awareness of these limitations and repeated supervised practice.
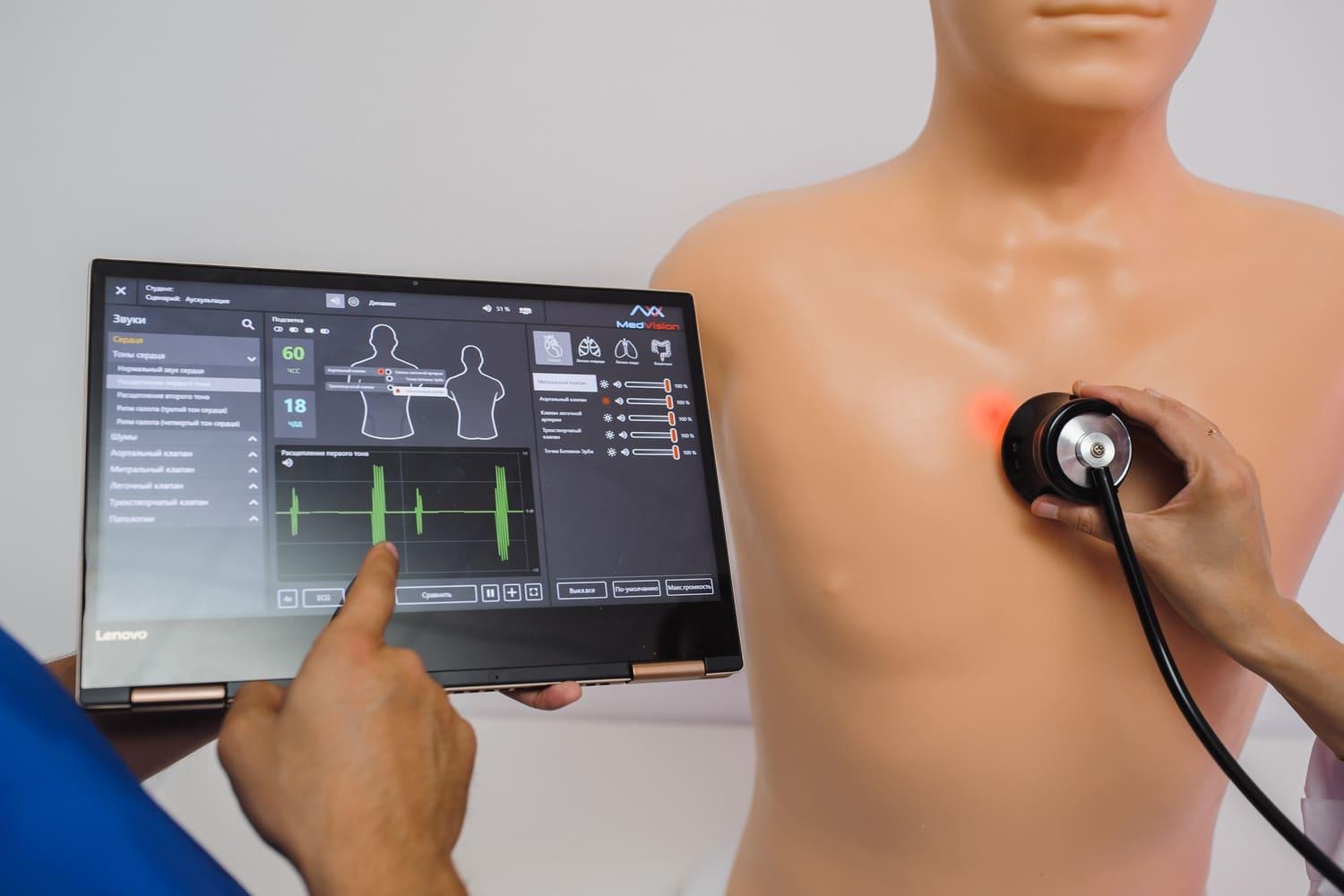
Digital auscultation and modern technology
Technological advances have introduced digital tools that enhance traditional auscultation. Electronic devices can amplify sound, filter background noise, and record acoustic findings for later analysis.
Digital auscultation supports structured education by allowing learners to replay heart sound and breath sound examples. This improves consistency in recognizing abnormal respiratory sound patterns.
Simulation-based systems such as MATT (Auscultation) and Pediatric MATT integrate realistic sound libraries into training scenarios, reinforcing standardized auscultation skills in controlled environments.
Auscultation in interdisciplinary clinical practice
Auscultation is not limited to physicians. It plays an essential role in nursing, emergency care, and primary evaluation settings.
Nurse auscultation is routinely performed to assess respiratory system stability, detect changes in lung expansion, and monitor heart sound during patient observation. Early detection of abnormal sound supports timely referral and intervention.
In interdisciplinary teams, shared understanding of auscultation findings improves communication and patient safety.
Standardization of auscultation skills in education
Training in auscultation skills follows structured frameworks. In medical school and nursing programs, learners are introduced to normal reference sound patterns before progressing to pathological examples.
Standardized simulation enhances exposure to rare or complex sound findings. Repeated listening sessions improve recognition accuracy and confidence in clinical reasoning.
Simulation platforms that reproduce realistic heart sound, breath sound, and combined respiratory patterns provide consistent practice opportunities that are difficult to achieve in routine clinical rotations.

Pediatric auscultation considerations
Auscultation in pediatric patients requires adaptation of listening technique. In children, heart sound frequency may be higher, and normal breath sound patterns differ from adults. The smaller thoracic cavity influences how sound travels through the body.
Developing pediatric auscultation skills involves recognizing age-specific respiratory sound variations. Simulation systems such as Pediatric MATT allow learners to train in identifying abnormal lung sound patterns within a controlled educational environment.
Auscultation in emergency settings
In emergency situations, auscultation is often performed rapidly to assess airway patency and cardiovascular stability. Immediate evaluation of breath sound and heart sound supports early clinical decisions.
Changes in sound intensity, asymmetry of lung expansion, or absence of respiratory sound may indicate critical conditions. In such scenarios, accurate auscultation skills contribute to rapid triage and stabilization within the acute care setting.
Auscultation in intensive care monitoring
In intensive care environments, repeated auscultation is integrated into continuous patient assessment. Although advanced monitoring devices provide numerical data, direct listening to internal sound remains clinically valuable.
In critically ill patients, subtle changes in respiratory sound or altered heart sound patterns may precede measurable deterioration. Structured nurse auscultation protocols ensure that bedside observations complement technological monitoring.

Correlation between auscultation and clinical reasoning
Auscultation is not limited to detecting isolated sound events. It forms part of a broader clinical reasoning process. Interpretation requires integration of patient history, physical findings, and systemic evaluation of the body.
For example, diminished breath sound combined with symptoms of dyspnea guides further investigation of the respiratory system. Likewise, abnormal heart sound may prompt imaging or laboratory testing. Strong auscultation skills enhance diagnostic pathways rather than replace them.
Objective documentation of sound findings
Modern practice encourages structured documentation of auscultation findings. Clinicians record the location, intensity, and character of each sound detected during examination.
Clear documentation supports continuity of care and allows comparison over time. In educational settings, standardized recording of heart sound, lung sound, and other respiratory findings reinforces systematic assessment habits developed in medical school.
Digital recording tools integrated into simulation platforms allow learners to review sound patterns repeatedly, improving retention and analytical accuracy.
References
- Laennec R.T.H. De l'Auscultation Médiate. Paris, 1819.
- Bickley L.S. Bates' Guide to Physical Examination and History Taking. Wolters Kluwer.
- Mangione S., Nieman L.Z. Cardiac auscultatory skills of internal medicine and family practice trainees. JAMA. 1997.
- Tavel M.E. Cardiac auscultation: a glorious past—and it does have a future! Circulation. 2006.
- Sarkar M. et al. Auscultation of the respiratory system. Annals of Thoracic Medicine. 2015.
Frequently Asked Questions
What is the purpose of auscultation?
The purpose of auscultation is to assess internal body function by analyzing sound produced by the heart, lung, and other organs. It supports early detection of abnormalities in the cardiovascular and respiratory system.
What organs are assessed during auscultation?
Auscultation is commonly used to evaluate the heart, lung, and abdominal organs. Each region produces characteristic sound patterns that assist in clinical diagnosis.
How can auscultation skills be improved?
Auscultation skills improve through repeated listening, structured education, simulation training, and supervised clinical practice. Exposure to varied sound examples enhances diagnostic confidence.
Immerse yourself in a demo to see how MedVision transforms traditional learning into an engaging, interactive experience
Subscribe for the Latest News!